OR in Healthcare Operations
Operations research in healthcare and operations research in workforce management are siblings — separated at birth, raised in different industries, solving the same mathematical problems under different names. Nurse scheduling is the other great set-covering problem. Patient flow through an emergency department is a queueing network with the same structure as a multi-skill contact center. Surgical scheduling is resource allocation under uncertainty with stochastic durations, just like contact routing with stochastic handle times.
The healthcare-WFM bridge matters because healthcare OR is far more heavily researched (thousands of papers, billions in funding) than contact center OR. Every advance in nurse rostering, patient flow optimization, or surgical suite scheduling has a direct analog in WFM — and vice versa.
Overview
Healthcare operations face the same fundamental tensions as WFM:
- Demand is stochastic. Emergency arrivals follow Poisson-like processes. Surgical durations are random. Patient acuity varies unpredictably.
- Capacity is constrained and expensive. Nurses, physicians, beds, and operating rooms are scarce. Over-provisioning wastes budget; under-provisioning endangers patients.
- Service quality is non-negotiable. A "service level" failure in healthcare is not an abandoned call — it can be a clinical outcome. The stakes are higher, but the optimization structure is identical.
- Scheduling is NP-hard. Nurse rostering with shift preferences, consecutive-day limits, skill requirements, and fairness constraints is the same combinatorial optimization problem as agent shift scheduling.
Mathematical Foundation
Nurse Scheduling as Set Covering
The nurse scheduling problem (NSP) minimizes staffing cost while ensuring each shift-period is covered:
where if nurse j is assigned to the roster, if nurse j's schedule covers shift-period i, is the coverage requirement, and is the cost.
This is a set covering problem — the same formulation used for contact center shift scheduling. The constraint matrix differs (nurse constraints include consecutive night shift limits, weekend patterns, clinical competency requirements), but the mathematical structure is identical. Column generation, the method that revolutionized airline crew scheduling, was independently adopted for nurse rostering (Burke et al., 2004).
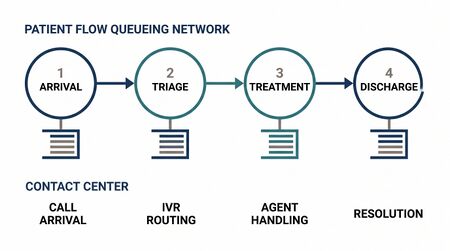
Patient Flow as Queueing Network
Patient flow through a hospital is a network of queues:
Arrival → ED Triage → ED Treatment → {Discharge, Ward, ICU}
Ward → {Discharge, ICU, Surgery}
ICU → {Ward, Discharge}
Surgery → {Recovery → Ward}
Each node is a queueing system with:
- Arrival rate (from external arrivals and transfers from other nodes)
- Service rate (treatment time, LOS)
- Number of servers (beds, nurses, physicians)
The network is analyzed using Jackson network results (if service times are exponential and routing is probabilistic) or simulation (for realistic distributions). The steady-state equations:
where is the total arrival rate at node i, is the external arrival rate, and is the routing probability from node j to node i.
This is structurally identical to a multi-skill contact center: channels (voice, chat, email) correspond to wards; skill groups correspond to clinical specialties; routing probabilities correspond to transfer rates.
Surgical Scheduling Under Uncertainty
Surgical scheduling assigns operations to operating rooms and time slots, subject to:
where is the (random) duration of surgery j, is the set of surgeries scheduled in slot t, and is the available time.
Because surgical durations are stochastic, the constraint is probabilistic:
This chance-constrained formulation is identical to WFM problems where service level must be met with probability given stochastic demand.
Parallel Structure
| Healthcare Concept | WFM Equivalent | Mathematical Connection |
|---|---|---|
| Nurse Scheduling Problem (NSP) | Agent Shift Scheduling | Same set-covering IP; same column generation approach |
| Patient acuity levels | Customer interaction complexity | Both drive variable service times and skill requirements |
| Nurse-patient ratios | Agent-occupancy targets | Both are capacity constraints expressed as ratios |
| ED patient flow | Multi-channel contact flow | Same queueing network; same routing optimization |
| Surgical duration uncertainty | Handle time uncertainty | Same stochastic programming formulation |
| Bed management | Workstation/seat management | Same capacity allocation under stochastic demand |
| Census-based staffing | Volume-based staffing | Both adjust capacity to current demand level |
| Clinical skill mix | Agent skill groups | Both require matching competencies to demand type |
| Triage (acuity-based prioritization) | Priority-based routing | Same multi-class queueing with priorities |
| Hospital readmission | Customer callback / repeat contact | Both indicate first-contact resolution failure |
| Length of Stay (LOS) | Handle Time (AHT) | Same metric: time from arrival to service completion |
| Patient satisfaction (HCAHPS) | Customer satisfaction (CSAT/NPS) | Same survey-based outcome measurement |
| Pandemic surge planning | Catastrophe / spike event staffing | Same capacity planning under extreme uncertainty |
WFM Applications
What WFM Can Learn from Healthcare
Acuity-adjusted staffing: Hospitals don't staff based on patient count alone — they staff based on acuity-weighted census. A ward with 20 low-acuity patients needs fewer nurses than one with 15 high-acuity patients. WFM can adopt this: weight staffing requirements by interaction complexity, not just volume. A queue with 100 simple password resets needs fewer agents than one with 60 complex billing disputes, even though the volume is lower.
Flexible staffing pools: Hospitals maintain float pools — nurses not assigned to a specific unit, deployable where census is highest. This is the exact model for cross-trained agent pools in WFM, and healthcare has 40+ years of research on optimal float pool sizing.
Fatigue and safety science: Healthcare has extensive research on the relationship between shift length, consecutive working days, and error rates. The Institute of Medicine's landmark report on medical errors directly linked nurse fatigue to patient safety. WFM can import these findings: extended shifts and consecutive working days degrade service quality in contact centers just as they degrade clinical quality in hospitals.
Discharge planning = Capacity liberation: In hospitals, delayed discharges block beds for incoming patients. The parallel: agents stuck in long after-call work or escalation queues cannot take new interactions. Healthcare's focus on "discharge planning" (active management of service completion) parallels WFM's focus on wrap-time optimization and escalation efficiency.
What Healthcare Can Learn from WFM
Real-time optimization: Contact center WFM has more sophisticated real-time management than most hospitals. Intraday reforecasting, automated VTO/VOT offers, real-time adherence monitoring, and automated schedule adjustments are standard in WFM but nascent in healthcare operations.
Workforce analytics: WFM's use of occupancy, utilization, shrinkage, and adherence metrics is more mature than healthcare's equivalent metrics. Hospitals can adopt WFM's interval-level analytics to manage nurse productivity with the same granularity that contact centers manage agent productivity.
Simulation for planning: Contact centers routinely use discrete-event simulation for capacity planning. Healthcare is adopting the same tools (Arena, Simul8, AnyLogic) but lags in systematic deployment.
Worked Example
Problem: Design a nurse scheduling system for a 30-bed medical unit using contact center column generation methods.
Setup:
- 24-hour operation, 3 shifts (Day 07:00-15:00, Evening 15:00-23:00, Night 23:00-07:00)
- Minimum nurse-patient ratios: Day 1:5, Evening 1:6, Night 1:8
- Staff: 25 nurses with varying availability, competencies, and preferences
- Constraints: maximum 5 consecutive days, minimum 2 weekends off per 4-week cycle, no more than 3 night shifts per 2-week period
Staffing requirements (census-based):
| Shift | Census Range | Required Nurses | Ratio |
|---|---|---|---|
| Day | 25-30 | 6 | 1:5 |
| Evening | 25-30 | 5 | 1:6 |
| Night | 25-30 | 4 (min 3) | 1:8 |
Column generation approach:
- Master problem: Select a set of roster patterns (columns) that covers all shifts at minimum cost
- Subproblem (pricing): Generate new roster patterns that improve the objective, subject to nurse-specific constraints
- Iterate: Solve the LP relaxation, generate columns, re-solve until no improving column exists
- Integerize: Apply branch-and-bound to the restricted IP
Result: The column generation approach produces a 4-week roster that:
- Meets all coverage requirements with 23 of 25 nurses (2 on leave)
- Satisfies all hard constraints (consecutive days, night limits, weekend allocation)
- Minimizes total premium pay (weekend and night differentials)
- Achieves 87% preference satisfaction (nurse shift requests honored)
This is exactly the same algorithm used by WFM platforms (NICE, Verint, Calabrio) for agent shift scheduling. The constraint types differ; the mathematical method is identical.
Pandemic Surge Planning
COVID-19 forced hospitals into the same capacity planning crisis that catastrophe events create for contact centers:
| Challenge | Healthcare Response | WFM Parallel |
|---|---|---|
| Demand surge (10x normal) | Cancel elective surgeries, convert wards | Cancel outbound, consolidate queues |
| Staff shortages | Travel nurses, redeployed specialists | Outsource overflow, emergency cross-training |
| Uncertain duration | Scenario planning (2 weeks, 2 months, 6 months) | Same scenario-based capacity models |
| Burnout and attrition | Hazard pay, mental health support, rotation | Same retention interventions |
| Resource allocation ethics | Crisis standards of care (triage protocols) | Prioritization rules for high-value customers |
Both domains used the same OR tools: simulation (to project capacity needs under scenarios), optimization (to allocate scarce resources), and queueing theory (to manage flow under extreme load).
Maturity Model Position
- Level 2 (Developing): Fixed staffing ratios; no queueing analysis of patient/contact flow
- Level 3 (Advanced): Census/volume-based variable staffing; basic scheduling optimization; awareness of healthcare-WFM parallels
- Level 4 (Leading): Acuity-adjusted staffing; column generation for rostering; queueing network analysis of flow; systematic cross-pollination of healthcare and WFM research
- Level 5 (Innovating): Integrated patient/contact flow simulation; real-time adaptive staffing borrowed from WFM; combined fatigue-quality models from healthcare safety science; AI-driven rostering with preference learning
See Also
- Column Generation in WFM
- Queueing Theory Fundamentals
- Constraint Programming in WFM
- Simulation in Workforce Management
- Operations Research in Workforce Management
References
- Burke, E.K., De Causmaecker, P., Vanden Berghe, G. & Van Landeghem, H. (2004). "The State of the Art of Nurse Rostering." Journal of Scheduling, 7(6), 441-499.
- Green, L.V. (2006). "Queueing Analysis in Healthcare." In Patient Flow: Reducing Delay in Healthcare Delivery, Springer.
- Cardoen, B., Demeulemeester, E. & Beliën, J. (2010). "Operating room planning and scheduling: A literature review." European Journal of Operational Research, 201(3), 921-932.
- Institute of Medicine (2004). Keeping Patients Safe: Transforming the Work Environment of Nurses. National Academies Press.
- Hulshof, P.J. et al. (2012). "Taxonomic classification of planning decisions in health care." Health Care Management Science, 15(3), 217-236.
