Healthcare Workforce Management
Healthcare workforce management applies workforce management principles — demand forecasting, staff scheduling, real-time management, and performance optimization — to clinical and non-clinical healthcare environments including hospitals, clinics, emergency departments, telehealth operations, and health plan contact centers.
Healthcare represents one of the most significant aperture expansions of WFM beyond the contact center. The domain shares the same fundamental challenge — aligning labor supply with variable demand — but introduces unique constraints: patient safety implications, clinical licensure requirements, mandatory staffing ratios, 24/7/365 coverage, and extreme demand variability driven by patient acuity, seasonal illness patterns, and unpredictable events.
How Healthcare WFM Differs from Contact Center WFM
While healthcare WFM and contact center WFM share the same DNA — forecast demand, schedule supply, manage in real time — the operational realities diverge sharply. Contact center WFM optimizes for service levels measured in seconds; healthcare WFM optimizes for patient safety outcomes measured in lives.
| Dimension | Contact Center WFM | Healthcare WFM |
|---|---|---|
| Demand unit | Contacts (calls, chats, emails) | Patients (admissions, visits, procedures) |
| Planning interval | 15–30 minutes | 4–12 hour shifts; daily census |
| Staffing model | Erlang C / simulation | Nurse-to-patient ratios; acuity-based staffing |
| Skill requirements | Product/channel skills | Clinical licensure (RN, LPN, CNA, MD); credentials; certifications |
| Regulatory constraints | Labor law; calling hours | Nurse staffing mandates; CMS conditions; Joint Commission; state licensure |
| Stakes of understaffing | Poor service level; customer dissatisfaction | Patient safety risk; adverse outcomes; regulatory violation |
| Demand variability | Seasonal, day-of-week, intraday patterns | Seasonal + unpredictable (flu season, pandemic, mass casualty) |
| Shrinkage | 25–35% | 20–30% (fewer meetings; more PTO/fatigue management) |
| Attrition | 30–45% | ~16% for RNs; but critical shortage makes each departure impactful |
| Schedule structure | Variable start times, part-time common | 12-hour shifts dominant; on-call rotations; weekend requirements |
| Credentialing | Minimal (product training) | State licensure, board certification, unit-specific competencies, ongoing CEUs |
The credentialing dimension deserves emphasis. In a contact center, a newly trained agent can typically handle any call within their skill group. In a hospital, a registered nurse certified in medical-surgical care cannot simply float to a neonatal ICU — the credential and competency requirements are legally and clinically binding. This makes workforce planning and shift design fundamentally more constrained in healthcare settings.
Nurse Staffing Ratios and Regulatory Requirements
Mandated Ratios
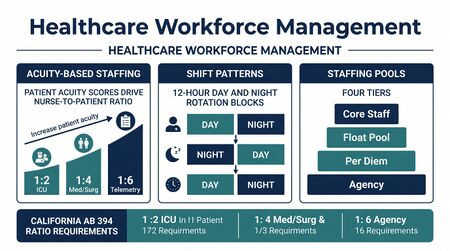
The most distinctive regulatory feature of healthcare WFM is mandatory nurse-to-patient staffing ratios. California's Assembly Bill 394 (1999, effective 2004) made it the first state to enforce specific numerical ratios for acute-care hospitals.[1] Key California ratios include:
| Unit Type | Maximum Patients per RN |
|---|---|
| Intensive Care (ICU) | 1:1 or 1:2 |
| Emergency Department (critical) | 1:1 |
| Emergency Department (general) | 1:4 |
| Medical-Surgical | 1:5 |
| Telemetry | 1:4 |
| Pediatrics | 1:4 |
| Labor & Delivery | 1:2 |
| Post-Anesthesia Care | 1:2 |
These ratios apply at all times, including during meals and breaks. Hospitals cannot assign unlicensed assistive personnel to perform RN functions to meet ratios.
Expanding State Mandates
Other states have followed California's lead, though approaches vary:[2]
- Oregon: Enacted comprehensive hospital minimum ratios effective June 2024 — ICU at 1:2, med-surg at 1:5 — enforced at all times including meals and breaks, with $200 penalties per missed break
- Massachusetts: Mandates 1:1 nurse-to-patient ratio in ICUs (since 2014)
- New York: Safe Staffing for Quality Care Act (2021, effective 2023) requires 1:2 in all ICUs and CCUs, plus on-call coverage requirements
- Federal: CMS released minimum staffing standards for nursing homes in 2024, requiring 3.48 hours per resident day (HPRD)
For WFM practitioners, mandated ratios function as hard constraints in the scheduling optimization — unlike contact center service levels which are targets, ratio violations carry regulatory penalties and patient safety consequences.
Staffing Committees
Many states that have not adopted numerical ratios instead require hospitals to establish nurse staffing committees. These committees — typically comprising at least 50% direct-care nurses — develop unit-specific staffing plans based on patient acuity, staff experience, and unit characteristics. This approach gives WFM teams more flexibility but requires robust data systems to demonstrate compliance.
Patient Acuity-Based Staffing Models
Mandated ratios set the floor, but effective healthcare WFM operates above minimums using acuity-based staffing — adjusting nurse assignments based on patient severity and care intensity.
Hours Per Patient Day (HPPD)
The core metric in healthcare staffing is hours per patient day (HPPD), calculated as total nursing hours worked divided by patient census. Average HPPD varies significantly by unit type — general medical-surgical floors average approximately 5.6 required RN hours per patient day, while ICUs may require 12–24 HPPD.[3]
Acuity Scoring Systems
Several classification systems drive acuity-based staffing:
- GRASP (Grace Reynolds Application and Study of PETO): One of the earliest and still widely used task-based systems in the US. Constructs a detailed care plan for each patient with timed tasks to determine required staffing
- Patient Classification Systems (PCS): Categorize patients into acuity levels (typically 1–4 or 1–5) based on clinical indicators — severity of illness, complexity of clinical judgment, need for specialized technology, and psychosocial factors
- Workload Acuity Tools: Newer systems that calculate real-time acuity scores per shift or per hour, enabling dynamic staffing adjustments
Acuity-based staffing represents the healthcare equivalent of capacity planning in contact centers — but instead of forecasting call volumes by interval, healthcare WFM forecasts nursing care hours by patient census and severity mix.
Scheduling Challenges
Healthcare scheduling is among the most complex in any industry, driven by overlapping constraints that far exceed typical employee scheduling scenarios.
12-Hour Shift Dominance
Most hospital nursing operates on 12-hour shifts (typically 7a–7p and 7p–7a), creating a fundamentally different shift design challenge than the variable-length shifts common in contact centers. Key implications:
- Fatigue management: Research consistently links 12-hour shifts to increased error rates after hour 10. Many states and collective bargaining agreements impose consecutive shift limits (e.g., no more than three 12-hour shifts in a row) and mandatory rest periods (minimum 8–11 hours between shifts)
- Weekend requirements: Most hospitals require nurses to work every other weekend, creating complex rotation patterns
- Holiday coverage: 24/7/365 operations require equitable holiday rotation across staff
On-Call and Float Pools
Healthcare organizations maintain several flexibility mechanisms analogous to contingent workforce models in contact centers:
- On-call staff: Nurses scheduled to be available but not actively working, called in when census exceeds forecast or staff call out. Typically compensated at a reduced "on-call rate" with premium pay when activated
- Float pools: Internal teams of cross-trained nurses who can work multiple units. Float pool nurses sacrifice unit specialization for scheduling flexibility and often receive premium pay differentials
- Per diem staff: Part-time nurses who work on an as-needed basis, providing schedule flexibility without agency costs
- Agency/travel nurses: External contract nurses filling longer-term gaps (see The Nursing Shortage and WFM below)
Self-Scheduling
Many healthcare organizations have adopted self-scheduling models where nurses select their own shifts within defined parameters. A typical self-scheduling workflow:
- Management publishes open shifts and coverage requirements
- Nurses submit shift preferences during an open enrollment window
- System or manager resolves conflicts and gaps
- Remaining gaps filled via float pool, on-call, or agency
Self-scheduling improves nurse satisfaction and retention but requires careful guardrails to prevent senior staff from claiming all desirable shifts while junior nurses absorb nights and weekends. Research published in JMIR in 2025 found that integrating nurse preferences into AI-based scheduling systems significantly improved schedule satisfaction scores.[4]
Forecasting Patient Census and Acuity
Healthcare demand forecasting parallels contact center forecasting but with distinct characteristics:
Census Forecasting
- Scheduled demand: Elective surgeries, clinic appointments, and planned admissions are predictable — similar to outbound campaigns in contact centers
- Unscheduled demand: Emergency department arrivals, trauma, and acute admissions are stochastic — similar to inbound call volume but with higher variance and lower predictability
- Seasonal patterns: Flu season (October–March), respiratory virus surges, and summer trauma increases create predictable seasonal demand curves
- Pandemic and surge events: COVID-19 demonstrated the need for surge capacity planning that far exceeds normal forecasting ranges
Acuity Forecasting
Beyond volume, healthcare must forecast the severity mix of incoming patients. A unit with 20 low-acuity patients requires fundamentally different staffing than one with 20 high-acuity patients. Advanced models incorporate:
- Historical acuity distributions by unit, season, and day-of-week
- Real-time admission data and diagnosis codes
- Transfer patterns from emergency department to inpatient units
- Post-surgical recovery trajectories
Length of Stay (LOS)
Unlike contact center interactions that last minutes, patients occupy beds for hours to weeks. Forecasting bed availability requires predicting discharge timing — a function of diagnosis, complications, insurance authorization, and social determinants (e.g., availability of post-acute care placement). LOS forecasting directly impacts next-day staffing requirements.
Technology Landscape
The healthcare WFM technology market includes specialized platforms, general HCM suites with healthcare modules, and point solutions for specific scheduling challenges.
Major Platforms
| Platform | Focus | Notes |
|---|---|---|
| UKG (Kronos) | Enterprise WFM | Leader in 2025 Gartner Magic Quadrant for Cloud HCM. Deep healthcare vertical with credential tracking, acuity-based staffing, and compliance management |
| symplr (API Healthcare) | Healthcare-specialized WFM | Acquired API Healthcare in 2019. Integrated workforce management with credentialing, compliance, and time/attendance |
| QGenda | Physician scheduling | Specialized in complex physician and advanced practice provider scheduling, on-call management |
| ShiftMed | On-demand nurse staffing | Technology-enabled marketplace connecting nurses with open shifts, reducing agency dependency |
| NurseGrid | Nurse scheduling/communication | Mobile-first scheduling platform focused on nurse experience and self-scheduling |
| Workday / ADP / Infor | General HCM | Enterprise platforms with healthcare-specific modules for time, scheduling, and compliance |
Maturity Gap
Despite the availability of sophisticated platforms, many healthcare organizations still operate at low WFM maturity. Spreadsheet-based scheduling remains common, particularly in smaller hospitals and physician practices — representing Level 1 maturity. The gap between available technology and actual adoption is wider in healthcare than in contact centers, partly because healthcare scheduling involves more stakeholders (nursing leadership, medical staff offices, compliance, union representatives) and more constraints.
The Nursing Shortage and Its WFM Implications
The US faces a structural nursing workforce crisis that makes WFM optimization existentially important for healthcare organizations.
Scale of the Shortage
- The Bureau of Labor Statistics projects over 193,000 RN openings annually through 2032[5]
- HRSA projects a shortage of approximately 78,610 full-time equivalent RNs by 2025, worsening to a 10% national shortage by 2027
- More than 1 million RNs are projected to retire by 2030
- Rural areas face a 22% shortage compared to 8% in metro areas (2026 projections)
- The licensed practical nurse (LPN) shortage is projected to reach 28%
Travel Nursing: Healthcare's Gig Economy
Travel nurses — temporary contract nurses placed by staffing agencies — represent healthcare's equivalent of contingent workforce models. The economics are stark:
- Hospital spending on travel nurses peaked at $44.6 billion in 2022 during the pandemic, dropping to an estimated $14.2 billion by 2025
- Hospitals pay 2.5–4x more per hour for travel nurses than permanent staff
- Average travel nurse bill rates were $89.78/hour in 2024, down from $106.63 in 2023
- Average weekly travel nurse pay was ~$2,300 in 2025, down 42% from pandemic peaks of ~$4,000
From a WFM perspective, travel nurse dependency is a cost signal of WFM failure — it indicates that an organization cannot match labor supply to demand through permanent workforce planning, scheduling optimization, and retention. Every dollar spent on travel nurses above permanent staff costs represents an opportunity for WFM improvement.
Burnout, Retention, and Schedule-Driven Attrition
Schedule-induced burnout is the central retention challenge in healthcare WFM. The connection between scheduling practices and nurse departure is well-documented:
- 39.9% of RNs report intent to leave the workforce or retire within five years, with 41.5% citing stress and burnout as the root cause[6]
- 52% of nurses feel so exhausted they dread facing another shift
- Average hospital RN turnover was 16.4% in 2024
- Nurse burnout affects an estimated 30–60% of nurses globally
Scheduling as a Retention Lever
Research consistently shows that scheduling practices directly predict retention outcomes. The most impactful turnover indicators for early-tenure RNs include joining teams where nurses consistently skip breaks and fail to take PTO — signals of chronic understaffing that WFM systems should detect and flag.
WFM-driven retention strategies include:
- Self-scheduling: Giving nurses control over their schedules improves satisfaction and reduces intent to leave
- Fatigue-aware scheduling: Algorithms that enforce rest periods, limit consecutive shifts, and flag overtime patterns before they become burnout drivers
- Equitable distribution: Ensuring nights, weekends, and holidays are distributed fairly rather than concentrated on junior staff
- Predictable scheduling: Publishing schedules further in advance (4–6 weeks versus 1–2 weeks) reduces stress and improves work-life integration
Telehealth and Virtual Care Impact
Telehealth has fundamentally altered healthcare workforce planning by decoupling certain clinical services from physical location.
WFM Implications
- Geographic flexibility: Nurses and physicians can provide virtual care from any location, expanding the available labor pool beyond local markets — analogous to the work-from-home revolution in contact centers
- Schedule flexibility: Virtual care shifts can be shorter and more varied (e.g., 4-hour blocks), enabling organizations to retain talent that might otherwise leave due to rigid 12-hour shift requirements
- Demand absorption: Telehealth triage can reduce in-person demand, smoothing workload for bedside staff
- Hybrid roles: Some organizations create hybrid positions combining virtual and in-person shifts, providing variety and reducing physical demands
- Specialized access: Virtual consults allow specialty providers to cover multiple facilities, reducing the need for on-site specialists at every location
The American Hospital Association reports that telehealth utilization has permanently shifted upward since 2020, with the global telehealth market projected to grow from $9.5 billion in 2024 to $85 billion by 2034. For healthcare WFM, this means building scheduling systems that accommodate both virtual and in-person care delivery — a blended workforce model.
AI and Machine Learning in Healthcare WFM
Artificial intelligence is transforming healthcare WFM across several domains:
Predictive Staffing
AI models analyze historical staffing patterns, seasonal patient trends, and real-time census data to forecast staffing needs days or weeks in advance. Key capabilities include:
- Census prediction: ML models that forecast patient volume by unit, shift, and acuity level
- No-show prediction: Identifying which scheduled staff are likely to call out, enabling proactive backfill
- Discharge prediction: Forecasting when patients will leave, improving next-shift staffing accuracy
- Surge detection: Early warning systems for demand spikes (e.g., respiratory illness clusters)
Scheduling Optimization
AI-powered scheduling goes beyond rule-based automation to optimize across competing objectives — coverage, cost, nurse preferences, fatigue limits, and credential requirements simultaneously. Mercy Health reported $30 million in savings in 2023 after implementing AI workforce management technology, with outcomes including reduced overtime, lower contract labor dependency, and improved nurse satisfaction.[7]
Documented ROI
Organizations implementing AI-driven healthcare WFM report:
- 10–12% decrease in labor costs through proactive, demand-based scheduling
- Reduced reliance on overtime and agency/travel nurses
- Improved schedule satisfaction scores among nursing staff
- Better alignment between staffing levels and actual patient acuity
The US AI in nurse scheduling software market is growing rapidly, driven by the convergence of the nursing shortage, rising labor costs, and increasing availability of real-time data from electronic health records (EHR) and nurse call systems.
Union Environments
A significant portion of the healthcare workforce — particularly in hospitals — is unionized. Union contracts introduce additional constraints on WFM:
- Seniority-based scheduling: Senior nurses may have contractual rights to preferred shifts and schedules
- Overtime rules: Mandatory overtime may be prohibited or subject to strict conditions
- Float restrictions: Contracts may limit which units a nurse can be floated to, reducing flexibility
- Schedule posting requirements: Minimum advance notice for schedule publication (often 4–6 weeks)
- Grievance processes: Schedule disputes may trigger formal union grievance procedures
WFM systems in unionized healthcare environments must encode these contractual rules as hard constraints in scheduling algorithms — a complexity layer that rarely exists in non-union contact centers.
Maturity Model Position
Healthcare WFM maturity can be assessed against the broader WFM maturity model, adapted for clinical environments:
- Level 1 (Reactive): Paper-based or spreadsheet scheduling. Staffing based on historical patterns and manager judgment. Heavy reliance on agency nurses for gap coverage.
- Level 2 (Foundational): WFM platform deployed. Automated scheduling with credential matching. Basic census forecasting. Float pool formally established.
- Level 3 (Integrated): Acuity-based dynamic staffing. Predictive demand models incorporating seasonal and diagnostic data. Float pool optimization. Self-scheduling for nurses. Integrated time/attendance and scheduling.
- Level 4 (Optimized): AI-powered demand prediction across units. Automated scheduling optimization balancing cost, coverage, preferences, and fatigue. Predictive attrition intervention. Agency spend reduction programs with measurable targets.
- Level 5 (Adaptive): Real-time census-driven staffing adjustments. AI-assisted triage and patient routing. Continuous workforce optimization with closed-loop feedback. Telehealth and in-person workforce managed as unified labor pool.
See Also
- Workforce Management — Overview of the WFM discipline
- Workforce Planning — Strategic workforce planning for healthcare talent
- Employee Scheduling — Scheduling principles applicable to healthcare
- Shift Design — Shift structure design including 12-hour shift considerations
- Labor Law and Scheduling Compliance — Regulatory compliance in scheduling
- Burnout and Schedule Induced Attrition — Schedule-driven burnout and retention
- Self-Scheduling and Flexible Workforce Models — Self-scheduling approaches used in healthcare
- GigCX and Contingent Workforce — Travel nursing as healthcare's gig model
- AI in Workforce Management — AI/ML applications in WFM including healthcare
- Capacity Planning Methods — Demand planning approaches adaptable to patient census
- Contact Center — WFM's original environment (comparison point)
- Forecasting Methods — Demand forecasting adapted for patient volumes
- Shrinkage — Healthcare-specific shrinkage patterns
- Attrition and Retention — Critical for nursing workforce
- Back Office and Knowledge Worker Workforce Management — Adjacent non-contact-center WFM
References
- ↑ National Nurses United. "California Safe RN-to-Patient Staffing Ratios." https://www.nationalnursesunited.org/california-safe-staffing-ratios
- ↑ NurseJournal. "Nurse-to-Patient Staffing Ratio Laws and Regulations by State." https://nursejournal.org/articles/nurse-to-patient-staffing-ratio-laws-by-state/
- ↑ PMC. "Acuity, Nurse Staffing and Workforce, Missed Care and Patient Outcomes." https://pmc.ncbi.nlm.nih.gov/articles/PMC7754324/
- ↑ JMIR Formative Research. "Integrating Nurse Preferences Into AI-Based Scheduling Systems: Qualitative Study." https://formative.jmir.org/2025/1/e67747
- ↑ Bureau of Labor Statistics. "Occupational Outlook Handbook: Registered Nurses." https://www.bls.gov/ooh/healthcare/registered-nurses.htm
- ↑ NCSBN. "Research Highlights: Small Steps Toward Nursing Workforce Recovery; Burnout and Staffing Challenges Persist." https://www.ncsbn.org/news/ncsbn-research-highlights-small-steps-toward-nursing-workforce-recovery-burnout-and-staffing-challenges-persist
- ↑ ShiftMed. "AI-Driven Predictive Staffing Analytics in Healthcare." https://www.shiftmed.com/insights/knowledge-center/ai-driven-predictive-staffing-analytics-healthcare/
